Description
Generic Name:
Semaglutide
Description:
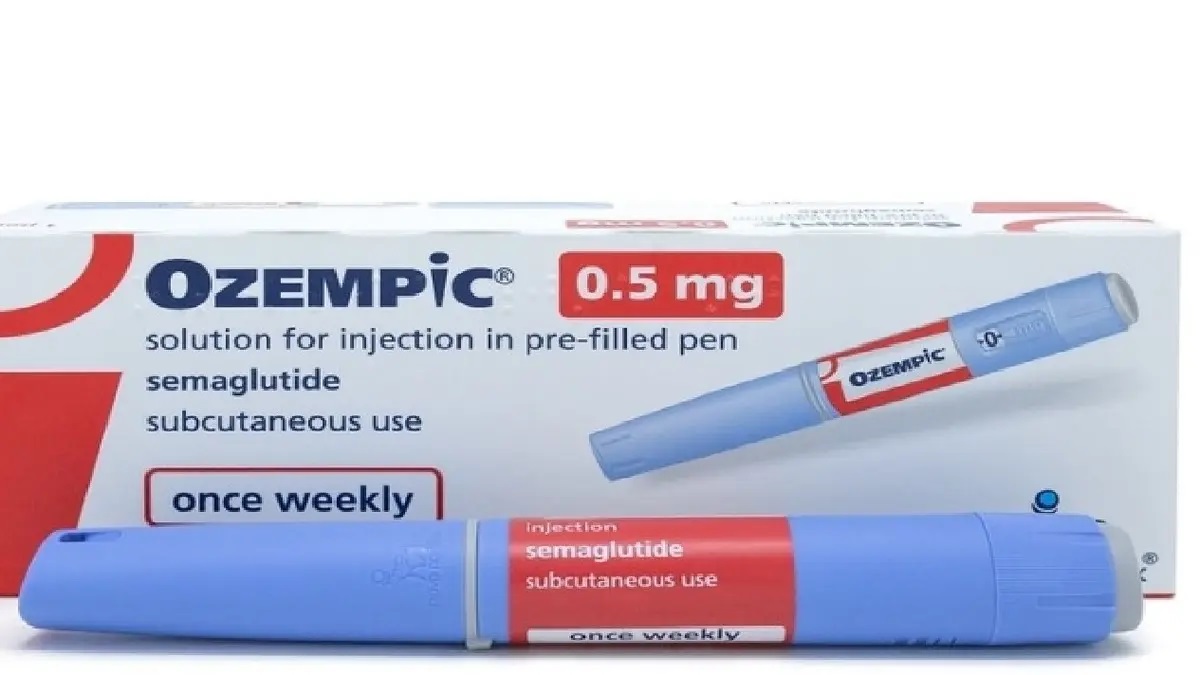
Ozempic (semaglutide) is a once-weekly injection that is FDA approved for use by adults with type 2 diabetes to control their blood sugar levels. Ozempic is also used by adults with type 2 diabetes who have heart and blood vessel disease to reduce their risk of a stroke, heart attack, or death. The active ingredient (semaglutide) in Ozempic has also been shown in clinical trials to be useful for weight loss, however Ozempic is currently not an FDA approved weight loss drug.
Ozempic is used when other medications have been tried but have not controlled the sugar levels well enough. It should be used along with a diet and exercise program.
Type 2 Diabetes is a long term condition when your blood sugars become too high as the body does not produce or use insulin normally. If you have high blood sugars over a period of time it can cause serious health problems including heart disease, stroke, kidney problems, nerve damage, and eye problems
Ozempic works to lower blood sugar levels by helping the pancreas to release the right amount of insulin when blood sugar levels are high, which moves sugar from the blood into other body tissues where it is used for energy. Ozempic injection also works by slowing the movement of food through the stomach and may decrease appetite and cause weight loss.
Ozempic injection is from a class of medications called incretin mimetics. Ozempic acts as a glucagon-like peptide (GLP-1) receptor agonist that selectively binds to and activates the GLP-1 receptor, the target for native GLP-1. GLP-1 is a hormone that has multiple effects on glucose, mediated by the GLP-1 receptors.
This medicine is not used to treat type 1 diabetes or diabetic ketoacidosis (a serious condition that may develop if high blood sugar is not treated). Ozempic is not used to replace insulin to treat people with diabetes who need insulin.
Indication :
Type 2 diabetes
Dosage:
Ozempic comes as a solution (liquid) in a prefilled dosing pen to inject subcutaneously (under the skin). It is usually injected once a week without regard to meals, on the same day each week at any time of day. You may change the day of the week that you use semaglutide as long as it has been 2 or more days (48 or more hours) since you used your last dose.
Your doctor will probably start you on a low dose of Ozempic and increase your dose after 4 weeks. Your doctor may increase your dose again after another 4 weeks based on your body’s response to the medication.
Ozempic can be injected into your upper arm, thigh, or stomach area. Change (rotate) the injection site with each injection. You can inject Ozempic and insulin in the same body area, but you should not give the injections right next to each other. Allow the pen to warm to room temperature before injecting if the pen was stored in the refrigerator.
Always look at the solution before you inject it. It should be clear, colorless, and free of particles. Do not use this medicine if it is colored, cloudy, thickened, or contains solid particles, or if the expiration date on the bottle has passed.
Follow the directions on your prescription label carefully, and ask your doctor or pharmacist to explain any part you do not understand. Use this medicine exactly as directed. Do not use more or less of it or use it more often than prescribed by your doctor.
Carefully read the manufacturer’s instructions for use that comes with the medication. These instructions describe how to inject a dose Ozempic . Be sure to ask your pharmacist or doctor if you have any questions about how to inject this medication.
This medicine helps to control blood sugar levels, but it is not a cure. Continue to use this medicine even if you feel well. Do not stop using this medicine without talking to your doctor.
Precaution & Warnings:
Ozempic injection may increase the risk that you will develop tumors of the thyroid gland, including medullary thyroid carcinoma (MTC) which is a type of thyroid cancer. Laboratory animals who were given semaglutide developed tumors, but it is not known if this medication increases the risk of tumors in humans.
Tell your doctor if you or anyone in your family has or has ever had MTC or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2) which is a condition that causes tumors in more than one gland in the body. If so, your doctor will probably tell you not to use this medicine. If you experience any of the following symptoms, call your doctor immediately: a lump or swelling in the neck; hoarseness; difficulty swallowing; or shortness of breath.
Prescription Information:
Proper doctor prescription is needed.
*Note: The prescription should not be older than 6 month.
Contraindication:
Ozempic can slow your digestion, and it may take longer for your body to absorb any medicines you take by mouth.
Tell your doctor about all your other medicines, especially insulin or other diabetes medicine, such as dulaglutide, exenatide, liraglutide, Byetta, Trulicity, Victoza, and others.
Other drugs may interact with Ozempic, including prescription and over-the-counter medicines, vitamins, and herbal products. Tell your doctor about all other medicines you use.
Tell your doctor and pharmacist what prescription and nonprescription medications, vitamins, nutritional supplements, and herbal products you are taking or plan to take. It is especially important to tell your doctor about all the medications you take by mouth because Ozempic may change the way your body absorbs these medications.



Reviews
There are no reviews yet.